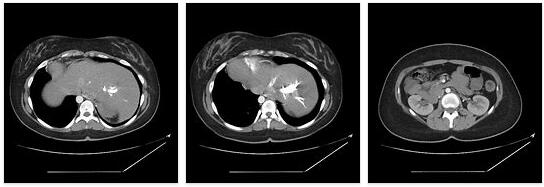
In the case of asplenia, the function of the spleen is disturbed or does not exist at all. This circumstance can be congenital or acquired. The spleen is an important organ in the human immune system as it is responsible for filtering certain pathogens in the blood. Usually, the body’s immune system can compensate for the lack of function of the spleen. However, asplenia patients are at greater risk of developing life-threatening sepsis due to bacterial, fungal, or parasitic infections. For this type of infection, these people should therefore be treated as soon as possible.
What is asplenia?
Asplenia is an inability of the spleen to function. The organ is also called Lien or Splen and is located in the left upper abdomen. The spleen consists of connective tissue through which blood constantly flows. The cells in this tissue pick up pathogens and old blood cells and destroy them.
This function is also called blood moulting. The organ has the task of filtering the blood in the human body. In anatmic asplenia, this organ is absent. This must be distinguished from what is known as functional asplenia, in which the organ is present but not functional.
Separate from this is the clinical picture of hyposplenia. Here the organ is laid out but its function is weakened. A splenectomy is surgical removal of the spleen. This may be necessary in certain diseases and circumstances such as tumors.
Causes
Anatomical, congenital asplenia is rare. Often the misalignment of the organ is related to congenital heart defects. This faulty system of the organ can be traced back to a midline defect. If a patient has both congenital asplenia and a heart defect, he or she will suffer from the Ivemark symptom complex.
This clinical picture can be assigned to the heterotaxies. Heterotaxia in general describes an innate rearrangement of human organs from one side of the body that is actually physiological to the other. The main symptom of the Ivemark symptom complex relates to a displacement, malformation or the absolute absence of the spleen.
The exact cause of this disease is not yet known. However, a genetic predisposition cannot be ruled out as it can occur more frequently within a family.
The so-called autosplenectomy is comparable to an anatomical asplenia. This can occur as a result of multiple splenic infarctions. These can be caused by bleeding or fibrosis. Fibroses are abnormal hardening of tissue that can lead to a functional disorder.
Functional asplenia must be differentiated from anatomical asplenia. This can result from autoimmune disease, stem cell transplants, sickle cell anemia, or amyloidosis. Sickle cell anemia is a hereditary disease that manifests itself as a reduction in the lifespan of red blood cells.
Amyloidosis is a pathologically altered deposit of proteins in the intercellular space. In sickle cell anemia in particular, functional disorders of the spleen usually occur after the first year of life. In the next few years, untreated patients will develop an anatomical asplenia caused by splenic infarction. Hyposplenia can develop in untreated HIV- positive people or after stem cell transplants.
Symptoms, ailments & signs
Asplenia patients are at a higher risk of infection. Certain bacteria, such as pneumococci, can cause serious blood poisoning. In addition, the risk of developing a fungal infection is increased.
American data from the 1980s also indicate that the risk of pneumonia and meningitis is higher for asplenic patients. People with asplenia suffer from decreased blood washing by the spleen and a decreased response of the immune system. Because of this, infections can pose dangerous risks for them.
In addition to pneumococci, asplenia patients due to meningococci and Haemophilus influenzae are particularly at risk of developing life-threatening sepsis. Your immune system cannot fight off these encapsulated bacteria as quickly as it can in healthy people. It is not only bacteria that can cause problems for asplenia patients. Parasites, tick bites, dog and cat bites as well as malaria can take a worse course in these patients than in healthy people.
Diagnosis & course
A blood test is used to diagnose asplenia. The so-called Howell-Jolly bodies are decisive here. These corpuscles usually contain nucleated red blood cells that are formed from DNA residues. Normally these bodies are broken down by the spleen.
In the case of asplenia, these can be detected in the blood because they are not filtered out of the blood due to the lack of or a functional disorder of the organ. Logically, patients with functional asplenia have lower Howell-Jolly scores than people with anatomical asplenia. The latter can also be recognized by imaging diagnostics such as ultrasound or computed tomography.
Complications
Various complications can arise due to asplenia. First, the inability of the spleen to function increases the risk of infection; Pneumococci and other capsule-bearing bacteria in particular can lead to serious health problems in asplenia. In less severe cases, the infections cause typical fever symptoms ; in severe cases, life-threatening sepsis occurs.
The risk of fungal infections also increases with asplenia. In addition, the inability of the spleen to function increases the risk of infections with Capnocytophaga canimorsus and other gram-negative pathogens that are transmitted, for example, through animal bites and tick bites. In addition, asplenia reduces the production of IgM antibodies and B memory cells; this can lead to increased diseases of the liver and infections of other organs.
Due to the impaired IgM antibody production, vaccinations also work much slower and less powerful, which increases the risk of diseases such as tetanus. The mortality rate with asplenia is around 46 percent, due to the wide range of complications and the many risks that an inoperable spleen brings with it. Early treatment and patient education can greatly reduce the risk of serious complications.
Treatment & Therapy
Normally, the body’s own immune system can protect the organism from pathogens even in the event of malfunctions or a lack of the spleen. However, the most important prophylaxis against serious complications is to vaccinate asplenia patients to protect them from bacteria and potentially life-threatening situations.
Vaccination against pneumococci, meningococci and Haemophilus influenzae are particularly important. In some cases permanent antibiotic treatment is induced. It is important to inform the patient comprehensively about his clinical picture during treatment.
If certain warning signs occur in a patient with asplenia, they should seek medical attention immediately. To do this, it is important that patients are trained on these signals. These include fever over 38 degrees Celsius, flu-like effects, confusion, racing heart, severe abdominal pain or dizziness.
Outlook & forecast
The prognosis for asplenia is very individual and depends on the patient’s health awareness. Basically, the stronger the health awareness, the better the prognosis. With a healthy lifestyle and regular participation in check-ups, the person affected has the opportunity to live their life without further impairments and without additional treatment measures. The lifetime is not shortened and a complete freedom from symptoms is possible.
The check-ups are necessary in order to identify possible pathogens in the organism at an early stage and to counteract them. The more unhealthy the patient’s lifestyle and the less he tries to get a medical check-up, the greater the risk of being attacked by germs.
These trigger diseases, the healing prospects of which have to be considered individually. Nevertheless, the immune system is weakened and can cause immense problems even with minor illnesses. The natural protection against the pathogens is not given in an asplenia. As soon as the person concerned neglects this, his own risk of illness increases.
In severe cases, he succumbs to an illness that his own immune system cannot cope with despite all efforts. It can then result in death. This occurs in particular if the participation in necessary protective vaccinations is not noticed and the pathogen is particularly aggressive.
Prevention
There are different causes for the clinical picture of asplenia. There are also various diseases that require the spleen to be removed. A safe prevention of this disease is therefore not yet given at the current state of knowledge.
Aftercare
Asplenia is considered incurable. Those affected therefore suffer from the inability of the spleen to function their entire life. The goal of follow-up cannot be to prevent the disease from recurring. Rather, it is about supporting patients in their everyday life and eliminating complications.
Asplenia can be diagnosed with a blood test. In addition, doctors regularly order a sonography and computed tomography for diagnosis. The patient himself has to take on a significant part of the follow-up care, such as adequate hygiene measures to prevent infection.
This includes, above all, avoiding crowds during the cold season. But careful hygiene after visiting public sanitary facilities is also important. If there are any initial signs of asplenia, the person affected must consult a doctor immediately. This is the only way to prevent complications. An early antibiotic therapy leads to an alleviation of the symptoms.
One of the most important preventive measures is to carry an emergency ID card with you, which lists the status of the vaccinations. Malaria areas should also be avoided when traveling abroad. If necessary, regular check-ups can be arranged with a doctor. In addition to discussing the state of health, blood tests play an important role.
You can do that yourself
Since the spleen is either absent or completely inoperative in asplenia, there are no methods that allow self-therapy for the underlying disease. However, patients can help manage the risks associated with asplenia.
The spleen plays an important role in the immune system of the human body. The spleen is particularly important for the defense against encapsulated bacteria, such as pneumococci, and for the defense against other parasites. People who suffer from asplenia therefore have a greatly increased risk of developing severe sepsis after a simple infection.
Prevention therefore has an important role to play. Situations that encourage infection with bacterial infectious diseases are dangerous for those affected. If possible, public transport and other crowds should be avoided during the cold season. Shaking hands should be avoided, as pathogens are transmitted particularly effectively. Regular hand washing can further reduce the risk of infection.
At the first signs of an infectious disease, such as a slight fever or unfounded exhaustion in connection with loss of appetite and shivering, the doctor should be consulted immediately so that treatment with antibiotics can be initiated as soon as possible. In addition, vaccinations can significantly reduce the risk of post-splenectomy sepsis.